Thymus Gland- Definition, Structure, Hormones, Functions, Disorders
The thymus gland is one of the key organs in the lymphatic system, which occurs in the mediastinum below the sternum.
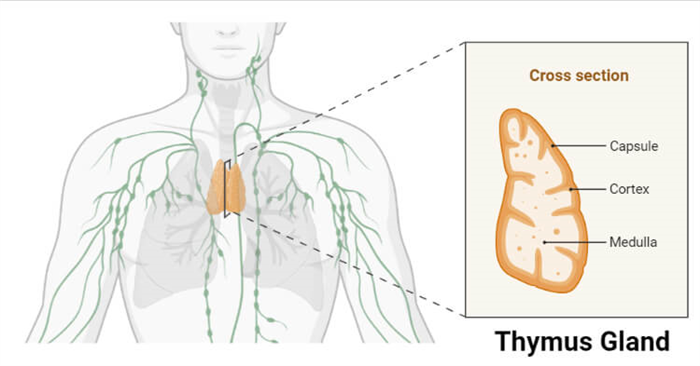
- The thymus extends from the lower edge of the thyroid gland to the fourth intercostal space of the vertebrae.
- The thymus gland is distinct from other endocrine glands in that it is active only before puberty. The gland grows the largest at puberty, after which the gland is slowly replaced by adipose tissue.
- The thymus gland is a critical organ of the immune system as it serves as a defense mechanism against different pathogens, tumors, and antigens.
- The thymus is particularly important for the thymus-dependent or adaptive arm of the immune system as the thymus is essential for the development and activation of immune cells.
- The term thymus is taken from Greek literature, where it means ‘soul’ to indicate that the soul resides in the thymus.
- In addition to the secretory cells of the thymus, it also contains other immune cells like macrophages, neutrophils, and dendritic cells.
- The proliferation of the secretory cells and the regulation of their secretions is maintained by cytokines like tumor necrosis factor (TNF) and interferon.
- The structure and function of the gland can be influenced by autoimmune diseases like myasthenia gravis.
Structure of Thymus Gland
- The thymus gland is a bilobed gland consisting of two pyramid-shaped lobes, each with a lobulated surface differentiated into the outer cortex and inner medulla.
- Each lobe of the gland is surrounded by a dense capsule of connective tissue and divided internally by a connective tissue septum.
- Most of the mass in the gland is occupied by a three-dimensional network of star-shaped reticular cells.
- The epithelial cells of the thymus gland are divided into four distinct subtypes depending on different factors like antigenic expression, ultrastructure, and their capacity to produce thymic hormones.
- The subtypes are subcapsular cortical, inner cortical, medullary, and Hassall’s corpuscles.
- The outer cortex of the gland contains loosely packed lymphocytes, and the medulla contains reticulocytes rich in the cytoplasm.
- The structure also contains small bodies called Hassall’s concentric corpuscles or Hassall’s bodies, or thymic corpuscles, which are concentric arrays of squamous cells.
- The size of the thymus is large in infants and young children, with the largest size at puberty. The gland then slowly begins to coalesce after puberty to be replaced by adipose tissue.
- The blood supply to the thymus gland is provided by the inferior thyroid, internal thyroid, and intercostals arteries.
- The gland is attached to the sternum by sternohyoid and sternothyroid muscles, both of which are bilateral.
Hormones of Thymus Gland
The thymus gland produces three different hormones; thymosin, thymopoietin, and the serum thymic factor. The thymic hormones do not act on the T cells identically. Their mode of action at the cellular level is based on the binding of the hormones to the specific cell receptors and the interaction with adenyl cyclase.
1. Thymosin
- Thymosin is produced by the epithelial cells of the cortex and medulla, and it is the primary hormone secreted by the gland.
- The most important function of thymosin is to induce T cell differentiation and enhance the immunological function of different immune cells.
- Thymosin has also been associated with increasing the phenotypic markers in lymphocytes.
- Thymosin is a protein that is heat stable up to 80°C temperature and might contain a small amount of carbohydrates.
2. Thymopoietin
- Thymopoietin is a polypeptide hormone of the thymus that has neuromuscular functions than immunological ones.
- However, the increased levels of the hormone are known to induce T cell activation and differentiation as well.
Functions of Thymus Gland
The following are some of the functions of the thymus gland;
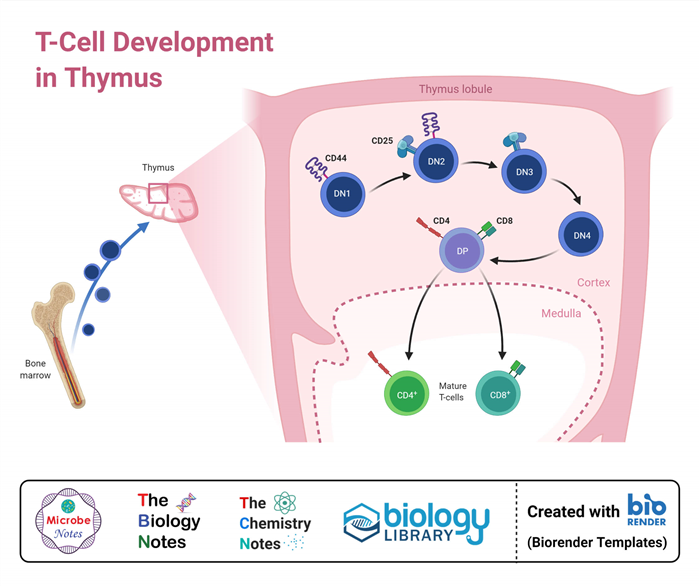
- The most important function of the thymus gland is to induce the development, activation, and differentiation of T cells so that they can perform their function as mediators of cellular immunity.
- The thymic hormones, thymosin, and thymopoietin stimulate the prothymocytes to become thymocytes and T lymphocytes.
- The gland also induces the release of cytokines that are essential for controlling the development of T cells through different stages.
- The thymus is a part of fetal immunity by the 12 th week of pregnancy and remains active through fetal life as well as childhood.
- As an endocrine gland, the thymus is known to produce human growth hormone, which is essential for the growth and development of the body.
Diseases and Disorders of Thymus Gland
The following are some of the disorders and diseases of the thymus gland;
1. Thymic cysts
- Congenital thymic cysts might be present within the thymus gland, resulting in the inhibition of proliferation of the thymocytes.
- These cysts can be removed and are usually benign. The individual with thymic cysts shows symptoms like cough and upper respiratory tract infections as the immune system of the individual is affected.
2. Involution
- Thymic involution is common in infants that are exposed to malnutrition, neglect, and abuse.
- Besides, it can also occur after chemotherapy, radiation, and steroid therapy as the thymus is sensitive to stress.
- Involution of the thymus is much rare in neonates, infants of early childhood.
- Premature involution can be taken as a symptom of social problems like abuse.
3. Hypoplasia
- Hypoplasia is the decreased number of cells in an organ, usually during neonatal conditions.
- Hypoplasia of the thymus occurs due to the development defect of the third and fourth pharyngeal pouches.
- It has been assumed that alcohol or organic acids tend to injure the neural crest that disturbs the differentiation of the pharyngeal pouch.
- The clinical manifestation of the condition depends on the extent of hypoplasia, and the amount of genetic material defected.